Non-small-cell lung cancer (NSCLC) accounts for more than 80 percent of lung cancer diagnoses and is the leading cause of cancer-related death worldwide. Current prognostication methods for NSCLC include techniques such as radiomics, which predicts the clinical outcomes (i.e. survival) based on the statistical characteristics of tumors in positron emission tomography-computed tomography (PET/CT) images, but their prognostic power is unsatisfactory.
To this end, University of Iowa College of Engineering researchers Stephen Baek, assistant professor of industrial and systems engineering; Xiaodong Wu, professor of electrical and computer engineering; and Yusen He, a PhD candidate in industrial engineering, along with their collaborators in Carver College of Medicine, recently published a groundbreaking new discovery in Scientific Reports, one of the top-ranked multidisciplinary research journals.
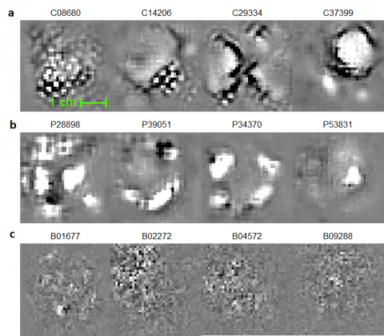
The UI researchers hypothesized that a deep convolutional neural network (CNN) algorithm trained for the automatic tumor segmentation task would develop abstract, high-level characterizations of tumoral and peritumoral geometry and that some of those abstract characterizations would be correlated with survival of NSCLC patients despite the fact that the AI algorithm had not been provided any survival related information. The UI team tested this hypothesis on 96 NSCLC patient data who received stereotactic body radiotherapy (SBRT) at the University of Iowa Hospitals and Clinics (UIHC) and discovered that some of the abstract characterizations of tumor geometry coded as numerical values in the CNN algorithm had remarkable prognostic power, leading to highly accurate survival prediction. The UI researchers confirmed the result through validation experiments conducted on 26 additional NSCLC cases with SBRT provided by the Stanford Cancer Institute, proving that the CNN-discovered biomarkers were generalizable and robust.
This result implies that physicians, in the future, might be able to accurately predict the survival of cancer patients for different cancer sites and different treatment options—the UI team's discovery is an important first step towards such a patient-tailored cancer treatment program.
More details on the team's discovery can be found here.